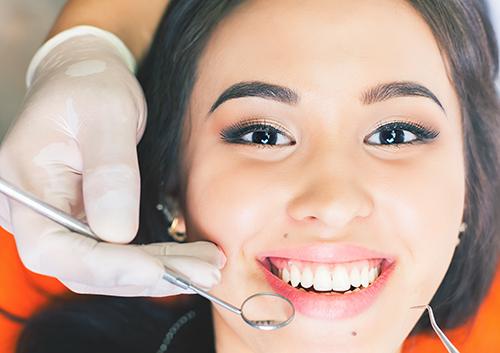
What is gum disease?
- posted: Apr. 23, 2024
Gum disease, also called periodontal disease, is an infection of the gum tissues, and is something seen all too often by the doctor. Extending from inflammation of the gums (gingivitis) Read More
Every Day is Earth Day
- posted: Apr. 16, 2024
During the early days of the environmental awareness movement, those who demonstrated against pollution, toxic chemicals, and the general public health were known as hippies. The early 1970s were a Read More
The Effects of Sleep Apnea on Dental Health
- posted: Apr. 09, 2024
Sleep apnea is an increasingly common medical condition, and one that can have a truly devastating effect on the waking life of the sufferer. Those who suffer from the disorder Read More
Snowball Effect
- posted: Apr. 02, 2024
Winter and its snowball fights are behind us, true, but there might be another kind of snowball heading your way—the snowball effect you risk when small dental concerns are ignored Read More
Dental Veneers
- posted: Mar. 26, 2024
Are you looking to improve the appearance of your front teeth? Dental veneers are widely used to improve the appearance of front teeth and are a much more conservative option Read More
What to do about Sensitive Teeth
- posted: Mar. 19, 2024
If you suffer from sensitive teeth, you already know the frustration of having a type of pain that is hard to deal with. Because tooth sensitivity is sometimes unpredictable, you Read More
St. Patrick's Day
- posted: Mar. 12, 2024
On March 17, everyone has a little Irish in them. St. Patrick’s Day is a joyous celebration of Irish heritage. The holiday originated as a commemoration of Saint Patrick, who Read More
Why do wisdom teeth need to be removed?
- posted: Mar. 05, 2024
Sometime around the late teens or early twenties, people’s wisdom teeth start to erupt. These are the third and final set of molars. When wisdom teeth come in properly — Read More
The Benefits of a Bright Smile
- posted: Feb. 27, 2024
Having a nice, bright smile can affect the way you look, and in turn, improve how you feel about yourself. With the help of the doctor to provide you with Read More
Medication Can Lead To Xerostomia in Women
- posted: Feb. 20, 2024
Xerostomia, otherwise known as dry mouth, can be a side effect of many common medications. Drugs used for blood pressure, birth control, antidepressants, or cancer treatments may cause the dry Read More
The Transformation of Valentine's Day
- posted: Feb. 13, 2024
Did you know the actions leading to the beginnings of Valentine's Day were actually centered on the avoidance of war? A Catholic priest named Valentine defied the orders of the Read More
Timing Matters!
- posted: Feb. 06, 2024
Many patients at Newmarket Dentistry are under the impression that harder brushing leads to cleaner teeth, but that is not true. Gentle brushing is just as effective, and less likely Read More
Breaking Bad Oral Habits
- posted: Jan. 30, 2024
The effects of bad oral habits are something our team sees all too often. You might have bad oral habits that stem from childhood, possibly because your parents did not Read More
Dental Filling Options
- posted: Jan. 23, 2024
You’ve made an appointment at our Newmarket, office to treat your cavity, the decayed area has been removed, and the site has been cleaned and prepared for a filling. Read More
Adult Mouthguards
- posted: Jan. 16, 2024
You make sure your daughter wears her mouthguard to every soccer practice. Your son doesn’t step on the basketball court without his. Why not protect your smile as well? Athletes of Read More
Common Causes of Gum Disease
- posted: Jan. 09, 2024
Your gums are responsible for a large part of your overall oral health. So keeping them healthy and knowing how to detect gum disease is extremely important. Since it’s often painless, Read More
This website includes materials that are protected by copyright, or other proprietary rights. Transmission or reproduction of protected items beyond that allowed by fair use, as defined in the copyright laws, requires the written permission of the copyright owners.